Medication Non-Adherence: The Elephant In The Room
“More health benefits worldwide would result from improving adherence to existing treatments than developing any new treatment.”
– WHO (World Health Organization), 2003
The high cost of non-adherence
Up to
$290B
cost to the US government¹
33-69%
unnecessary hospital admissions²
2x higher
mortality rates³
Up to
$290B
cost to the US government¹
33-69%
unnecessary hospital admissions²
2x higher
mortality rates³
1. Cost in avoidable hospitalizations, emergency care and outpatient visits due to poor patient adherence.
2. Result of non-adherence (in the US).
3. For patients with diabetes and heart disease who don’t adhere to medications as compared to those who do.
Patient persistence consistently less than 50%
Across disease states, patients struggle with persistence on medication. This is even lower in minority populations. The odds of non-adherence to antihypertensive medications were 47% & 44% higher among Black & Hispanic patients, as compared to white patients.
Lower medication adherence among Black and Brown communities is not limited to one or a few health conditions — these disparities have been demonstrated in communities of color across a wide array of diseases.
Source: PhRMA: Addressing Disparities in Medication Access and Adherence, May 2022
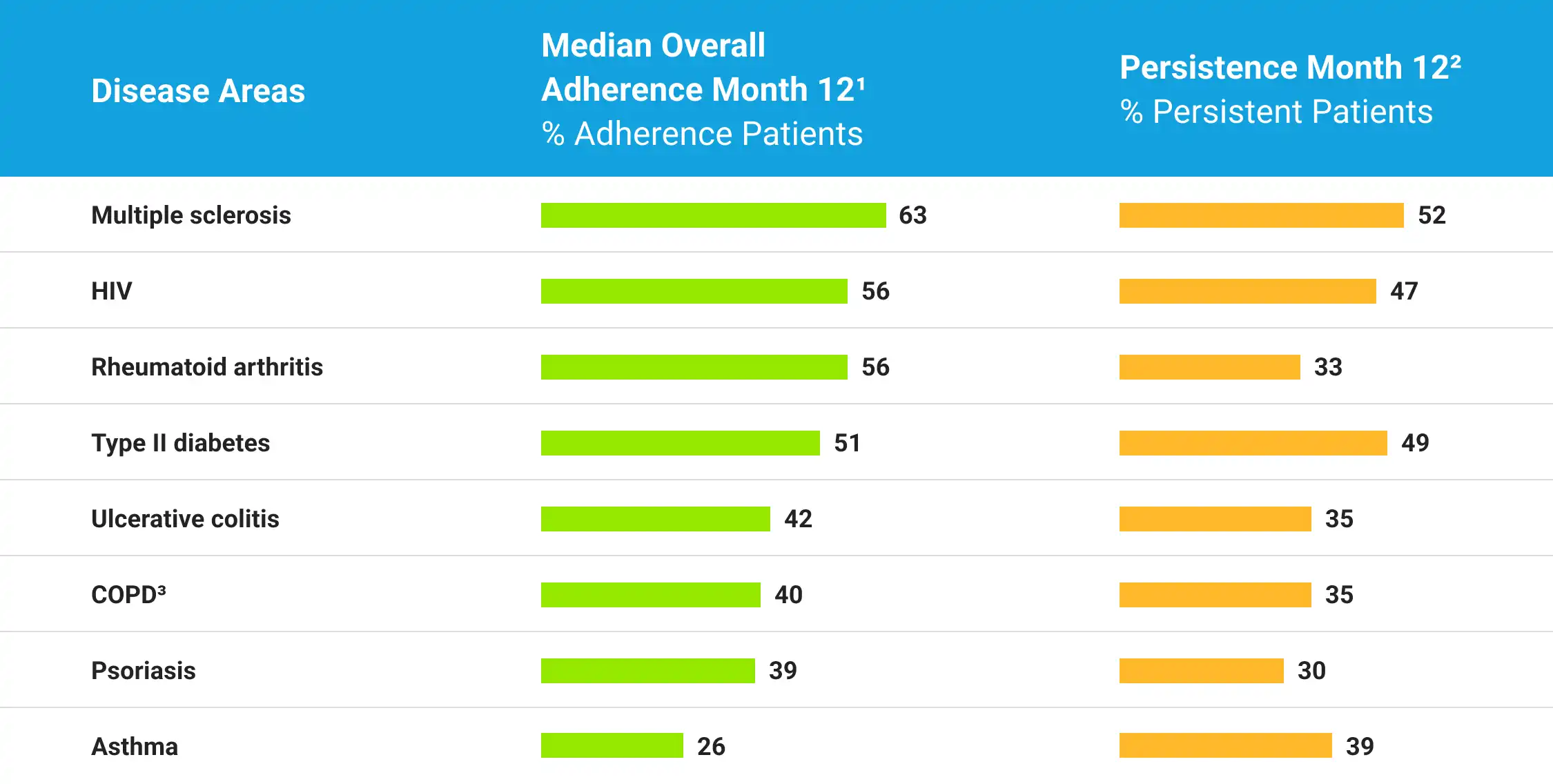
1. Calculated by averaging the 12-month values for each drug within each therapeutic area.
2. Percentage of patients who are fully adherent (>80% overall adherence) after 12 months.
3. Chronic obstructive pulmonary disease.
Source: PhRMA: Addressing Disparities in Medication Access and Adherence, May 2022
The challenge
“Drugs don’t work in patients who don’t take them.” –C. Everett Koop, former Surgeon General
Living with a serious disease can be overwhelming. Despite best efforts, patients struggle to take their medication as intended: doses get missed, refills get delayed, or treatment stops entirely. Unfortunately, it takes about ten weeks to establish a new habit and only one week to lose it.
Traditional approaches to helping patients start and stay on their medication don’t work because they add to the burden or act too late. Oftentimes, these approaches are driven by dated prescription refill data and arrive when the medication-taking behavior has been broken. Newer methods, such as digital apps, suffer from low uptake and have no insight into the patient’s life arriving too late or too often, resulting in alert fatigue and patient disengagement.
1. Can the theory of planned behavior predict the maintenance of physical activity?
2. How are habits formed: Modelling habit formation in the real world
The solution
Adherence = Retention + Compliance
Aidia is the in-home partner which effortlessly integrates into a patient’s life. An elegantly simple and proven system designed to gently remind people to take their medications and intervene when they don’t — early enough to make a difference. Making sure not a day is lost on their path to better health.
Real-time reinforcement
Aidia makes medication- taking behavior visible to the patient, helping form a positive reward cycle.
Personalized messaging
Aidia provides personalized messaging via SMS & voice, using data to identify key touchpoints across the patient journey.
Targeted Intervention
Real-time monitoring of patient behavior helps drive targeted intervention and coordination with care teams before it’s too late.
The results
50% +
avg increase in patient retention on medicine at 1 year
+3
additional prescriptions at 1 year
10:1 ROI
est. for pharma manufacturers after 1 year
(based on high priced specialty medications)
50% +
avg increase in patient retention on medicine at 1 year
+3
additional prescriptions at 1 year
10:1 ROI
est. for pharma manufacturers after 1 year
(based on high priced specialty medications)
Data sources available upon request.